After just 2 hours of intervention, doctors at Vietnam National Children’s Hospital successfully performed transcatheter pulmonary valve replacement (TPVR) for L.V. (14 years old, Nghe An). About 30 minutes later, the patient was awake, weaned off mechanical ventilation, and did not have to undergo a second open-heart surgery with repeat sternotomy.

Only a few days after the procedure, L.V. was able to return to normal daily activities, with no more shortness of breath or fatigue.
Previously, the possibility of re-operation had caused significant anxiety for the family. “Doctors warned that a second surgery might be needed to replace the pulmonary valve… Thinking about my child having the sternum cut open again made me extremely worried,” the child’s father recalled.
13 years after Tetralogy of Fallot repair: pulmonary valve function declines over time
L.V. was born with a complex congenital heart defect—Tetralogy of Fallot (TOF)—and underwent complete repair at 1.5 years of age. After surgery, the child developed well, lived normally, and attended regular follow-up visits. Recently, the child developed chest pain, shortness of breath, fatigue, and episodes of fainting. Echocardiography and cardiac MRI showed severe pulmonary valve regurgitation, with blood flowing back into the right ventricle.

Treatment options: repeat open-heart surgery vs. transcatheter valve replacement
Two options were considered:
- Repeat open-heart surgery to implant a new valve: the traditional approach, with lower cost, but it is major surgery requiring sternotomy, temporary cardiac arrest, and incision of the pulmonary artery to place a new pulmonary valve. Re-entry surgery also requires dissection through scar tissue from the previous operation, increasing the risk of bleeding, complications, and a longer recovery period.
- Transcatheter pulmonary valve replacement (TPVR): a less invasive option that avoids repeat open-heart surgery. A prosthetic valve mounted on a metal stent is compressed within a catheter and delivered through a major blood vessel in the groin (femoral access) to the site of the leaking pulmonary valve. The valve is then deployed and begins functioning like a normal valve.

Coronary compression risk: careful planning with VR imaging and international expert consultation
Despite being minimally invasive, this case carried a high-risk anatomical feature: the child’s left coronary artery was located very close to the pulmonary artery. Dr. Cao Viet Tung explained: “The greatest risk is that the prosthetic valve could compress the coronary artery after deployment, causing acute myocardial ischemia—potentially life-threatening during the intervention.”
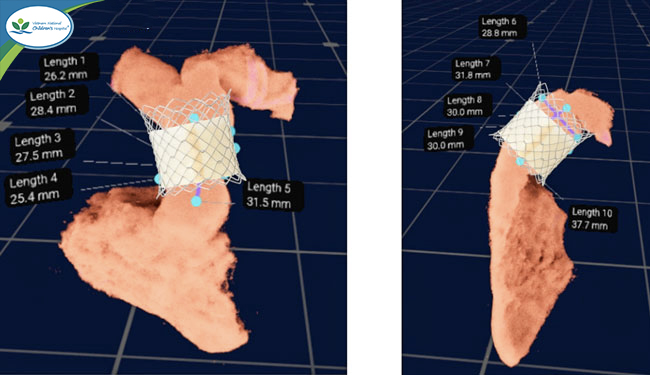
To ensure safety, the team consulted with experts from Seoul National University and Children’s HeartLink. In addition, physicians used Virtual Reality (VR) technology based on multislice CT data to reconstruct a 3D model of the right ventricle and pulmonary artery. The model could be rotated 360 degrees, enabling accurate anatomical assessment and helping determine:
- the safest valve implantation position, and
- the appropriate valve size for the patient.
Rapid recovery: no second sternotomy required
The intervention lasted approximately 2 hours. The pulmonary valve was delivered via the femoral vein. Under the guidance of digital subtraction angiography (DSA) combined with roadmapping, the valve was positioned accurately, deployed successfully, and functioned immediately like a natural valve—without coronary artery compression.
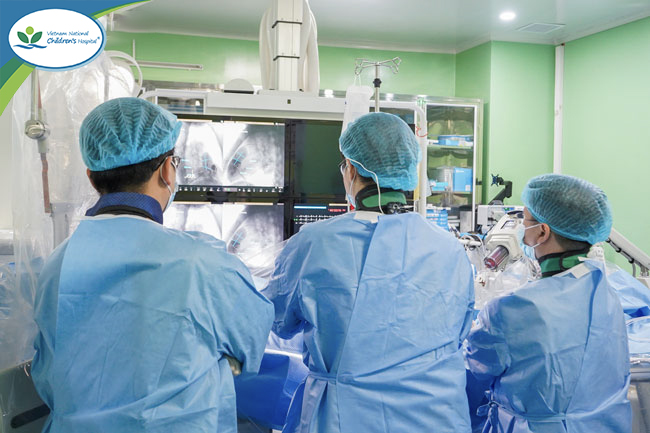
DSA imaging supported the precise localization of the implantation site.
About 30 minutes after the procedure, the patient woke up, was weaned from mechanical ventilation, and the endotracheal tube was removed. The patient is currently stable, with no shortness of breath or chest tightness. Echocardiography shows good valve function and no evidence of coronary compression.

Transcatheter pulmonary valve replacement is a modern treatment trend that reduces the need for repeat surgery in patients after complete TOF repair. This successful case highlights the effectiveness of combining clinical expertise, international consultation, and advanced imaging technology to deliver individualized treatment. For children who have undergone heart surgery at an early age, TPVR can reduce trauma, shorten recovery time, and improve quality of life.
|
Tetralogy of Fallot is a complex congenital heart defect involving four structural abnormalities, often referred to as cyanotic congenital heart disease. It is characterized by reduced oxygen delivery, causing cyanosis, fatigue, and delayed growth. Timely surgery is required to prevent cardiovascular complications or death from acute hypoxic spells. Each year, Vietnam National Children’s Hospital successfully performs surgery for approximately 100 children with Tetralogy of Fallot. However, even after complete repair, patients may still face long-term complications such as pulmonary valve regurgitation, right ventricular dysfunction, arrhythmias, residual pulmonary stenosis, or residual ventricular septal defects. |
Digital Information Office – Training and Research Institute for Child Health



